What’s New

On Wednesday, December 6, 2023, from 8:00 AM to Noon, IBHI will offer its annual, well-received seminar on Improving Emergency Department Flow for People with Behavioral Health Problems at the Paris Las Vegas Hotel & Casino, Las Vegas, NV, preceding the 14th Annual National Update on Behavioral Emergencies Conference at the same location. Read more here.
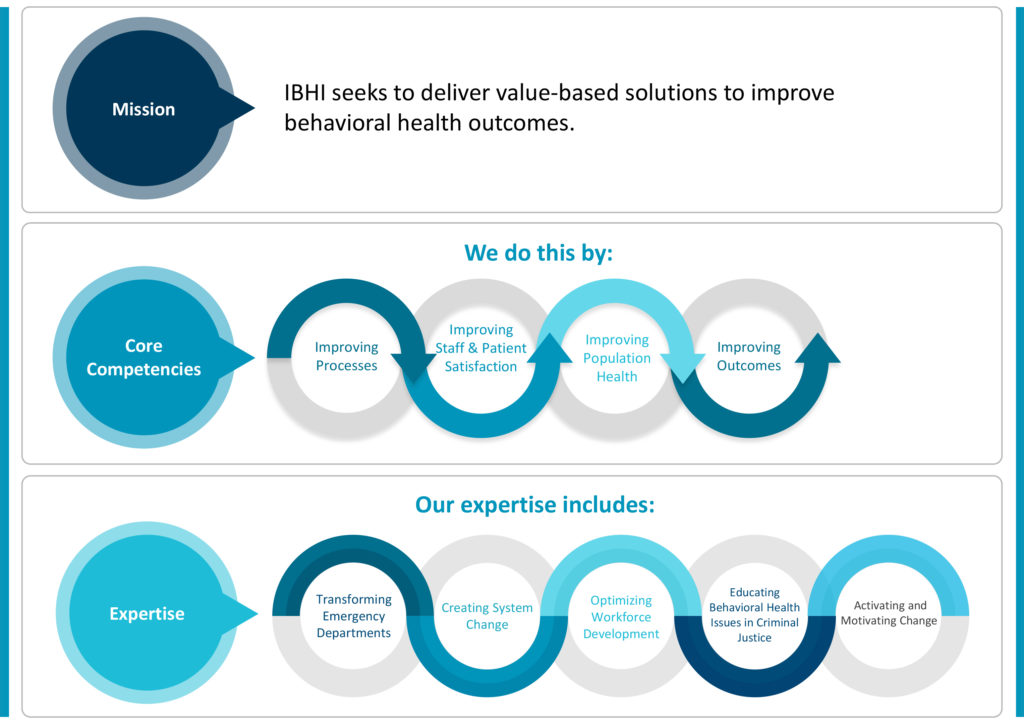
The Institute for Behavioral Healthcare Improvement (IBHI)
was formed in 2005 when the founding members, along with leaders in behavioral health and healthcare quality, recognized the need to create a more robust, effective quality improvement processes within behavioral healthcare. IBHI decided to emulate the general health care platform created by the Institute for Healthcare Improvement (IHI) but with the primary focus on behavioral health care. As a result, the primary mission of IBHI is to dramatically improve behavioral health care outcomes by creating a high performing national learning organization that invites organizations out of their historical silos. IBHI seeks to encourage a movement that translates a passion for quality improvement into sustained action.